
Performing Cataract Surgery
For Over 35 Years


Cataract surgery is the most common surgery performed in the U.S. today. It is performed on an out-patient basis and can offer significant improvements to vision. In cataract surgery, the clouded lens of your eye is replaced with a plastic lens, an intraocular lens (IOL). Dr. Levinson has performed over 6,000 Cataract Surgeries.
Click title to read details…
What are cataracts?
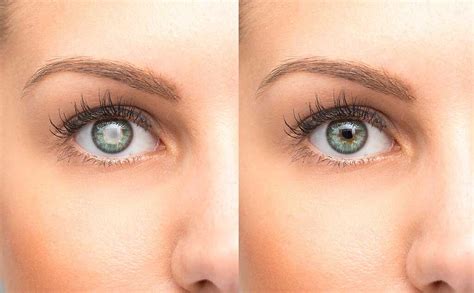
Cataracts are a slowly-progressing discoloration of the lens of the eye that probably actually starts the day we are born. The lens is crystal clear at birth but slowly turns brown with age, mostly due to UV-induced changes in the proteins of the lens. Everybody’s lens discolors with age but not everybody needs cataract surgery. Eventually, the brown discoloration of the lens may interfere with vision and that’s when you need cataract surgery.
When do you need cataract surgery?
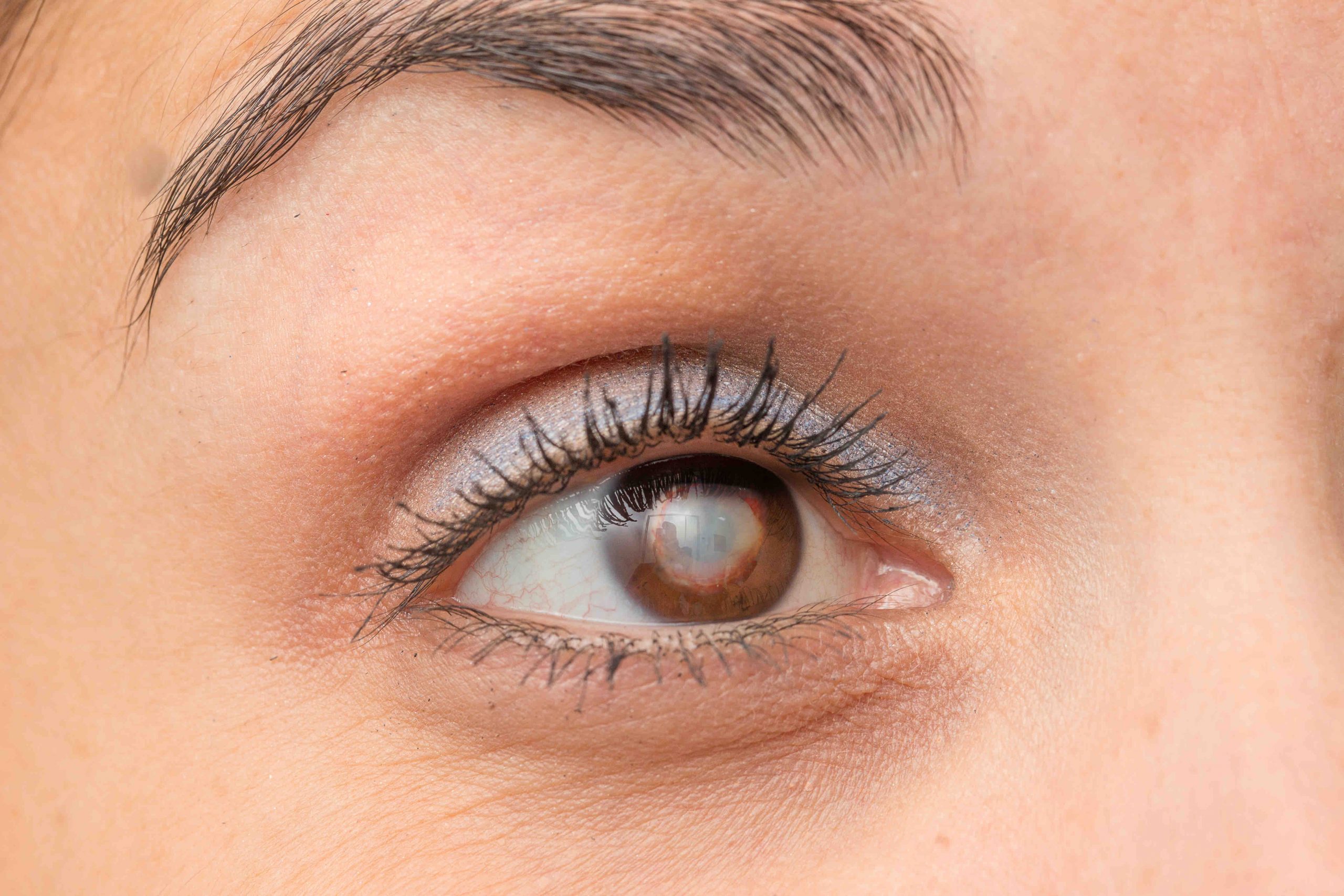
Cataract surgery is elective. You have cataract surgery when your lens has discolored to the point that you are having difficulty seeing to perform your daily activities. Typical cataract-induced vision complaints are glare in bright light or at night from headlights, blurred, dim or distorted vision. The cataract does not physically damage the eye but it sure can blur the vision. When you are having difficulty seeing to do your daily activities, like driving, especially at night, reading, seeing to walk safely, etc., then you need to consider cataract surgery.
Obviously, if you are having difficulty seeing to perform your daily activities, you need to have your eyes examined. Cataracts aren’t the only cause of blurred vision. You may just need your glasses prescription updated, or you may have other problems with your eyes, like glaucoma, macular degeneration, dry eye, etc.
Cataract surgery.
During cataract surgery, a small, self-sealing 1/8 inch incision is made in your eye’s cornea – the clear, outer layer of your eye. The wound is so small it does not even usually require a suture to close. The lens of your eye is removed and an intraocular lens (IOL) is inserted in its place. The IOL is not susceptible to discoloring like your original lens. You may feel pressure during your cataract surgery, but the majority of patients do not describe the procedure as painful. Anesthetic eye drops are administered to numb your eye.
IOL (Intra-Ocular Lens) options.

The primary goal of cataract surgery is to remove the old, hazy lens in your eye and to replace it with a new, clear artificial lens, to improve your vision.
When selecting the new lens, called an intraocular lens (IOL), surgeons have literally thousands of different IOL designs and powers from which to choose.
We have the opportunity to select a lens to insert that, if you like, can significantly decrease your dependence on glasses. The challenge with having so many different IOL options is to help you decide which option can best meet your needs and expectations. If you don’t mind wearing glasses after your cataract surgery, the IOL choices are relatively simple. If, however, you are interested in decreasing your dependence on glasses after cataract surgery, the options increase significantly. There is not a perfect IOL that focuses perfectly for all distances, like the natural lens in a young, healthy eye. However, there are IOLs available that may be effective in decreasing your dependence on glasses, allowing you to see well enough to pass a vision test for a driver’s license, to see your computer and/or to read menus, books, etc. without glasses. The IOL options we have can be effective at decreasing your dependence on glasses, but they are not perfect. To get your sharpest vision possible, you may still need to wear glasses. Here are the options:
Intraocular Lens Implant (IOL) Options.
———————————————————————–
1. Set eye for distance vision, or for near vision.
Pros:
• No premium charges for a traditional IOL.
Cons:
2. Monovision- Set dominant eye for distance and non-dominant eye for near.
Pros:
• No additional fees for this traditional IOL.
Cons:
3. Panoptix Multifocal IOL.
Pros:
• Corrects astigmatism, if necessary.
Cons:
4. Vivity Multifocal IOL.
Pros:
• Corrects astigmatism, if necessary, at no additional cost.
Cons:
5. Toric IOL to correct astigmatism, if needed.
Pros:
• Can significantly correct astigmatism.
Cons:
6. Light Adjustable IOL.
The Light Adjustable Lens (LAL) can be fine tuned after it has been inserted in your eye, allowing us to maximize your potential for your best uncorrected vision. The LAL has a “macromere,” a molecule that expands when exposed to UV light, imbedded in the IOL material. This IOL can be adjusted after being inserted in your eye by a customized application of UV to the IOL, specific for your eye by a laser-like scanning device, to fine tune the IOL correction.
This IOL is especially recommended for people who have had prior LASIK, PRK or RK surgery because this group of patients have an increased risk of unpredictable residual refractive error (prescription), especially astigmatism, after cataract surgery. The LAL is also recommended for patients that want to attain the best possible uncorrected vision possible with present-day technology. Unpredictable refractive error can be effectively minimized by adjusting the Light Adjustable IOL approximately 3-6 weeks after surgery. After the LAL is adjusted, the prescription is “locked in” to the LAL to finalize and stabilize the LAL prescription. The Light adjustable IOL is a monofocal lens that can be set for either distance, intermediate, or near vision.
Pros:
Cons:
IN SUMMARY:
In my experience, I’ve had the most success in decreasing dependence on glasses, with the fewest uncorrected and uncorrectable vision complaints after cataract surgery, by implanting an IOL for distance in the dominant eye and the Vivity multifocal IOL for intermediate and near vision in the non-dominant eye.
The advantage to this combination is potentially good distance, computer, and reading vision without significant night glare and halos.
However, no matter which IOL option you select, you may still need to wear glasses for night driving, TV, movies, computer and/or reading. No combination of IOL implants is perfect, but we do have options that allow most patients to function with the least need for glasses or the least risk of debilitating and uncorrectable glare and halos for night driving. And no matter which option you select, there is a 1-2% chance you’ll be very unsatisfied with your vision and will need the IOL removed and replaced with a different IOL option.
Obviously, the choices available can be confusing and overwhelming. I’m happy to discuss all options with you to help you clarify your needs and your realistic expectations, and to help you choose which option may work best for you.
What causes cataracts?
The human lens is mostly made of protein and water. With aging, the proteins in the lens discolor, turning the lens brown, causing what we call a cataract. Diabetes and chronic steroid usage can further increase cataract formation. The increasing discoloration of the lens is similar to a dirty windshield on your car, especially in the winter when slush drys on the windshield. With increasing “dry slush on your windshield”, light entering the eye is scattered by the cataractous lens, causing the patient to experience haze, glare and distortion, ie blurred vision. Changing your glasses prescription will not improve blurry vision caused by cataracts. Cataracts tend to progress but at an unpredictable rate. There is no known, scientifically verified treatment or supplement that prevents cataract formation. Everybody develops cataracts with aging and about 75% of people eventually have cataract surgery.
How are cataracts treated?
If your cataract is affecting everyday tasks like walking, driving and reading, or if it is interfering with your quality of life, you should have the cataract removed. Cataract surgery is the only effective way to eliminate cataracts. Cataract surgery removes the clouded eye lens and replaces it with an intraocular lens.
Is cataract surgery risky?
Cataract surgery is one of the most common surgeries performed today. It does carry the risk of certain complications, but it also has an excellent record of safety and a low rate of complications. Most estimates say that less than 5 percent of patients will experience serious complications. Most of those complications are treatable. Certain factors increase the risk of serious complications, such as the presence of other eye diseases. Dr. Levinson will discuss all the risks of cataract surgery with you during your pre-op examination.
What happens during cataract surgery?
First, a tiny incision is made in the cornea – the clear, curved outer portion of your eye. The lens is dissolved with ultrasound energy, called phacoemulsification, and the residual small lens fragments are removed from the eye with suction. An intraocular lens (IOL) is then inserted in the eye. The IOL is held in position by the same lens capsular that held your previously removed cataractous lens. There are no sutures involved in fixating the IOL.
What to Expect from Cataract Surgery
Cataract surgery is the most commonly performed surgery in the US. Cataract surgery has an extensive safety record, and serious complications are rare and usually treatable. In my practice, 97% of cataract surgeries are without complication.
After your surgery, you may experience:
• Itchy eyes
• Dry eyes
• Blurry vision
• Mild discomfort
• Discharge from your eyes
Most patients can return to normal daily activities within 24 hours after cataract surgery with only minimal restrictions. Your vision may continue to adjust to the IOL for a month or so, and you may want to use reading glasses during this time. After about a month, your eyes and vision should adapt to the IOLs. If you need glasses to fine tune your vision, the glasses are typically prescribed 3-4 weeks after surgery.
The blurriness and poor vision caused by a cataract can be devastating and can interfere with your day-to-day activities. If a cataract is affecting your ability to drive, read and enjoy life, cataract surgery may be right for you.
To learn more about Denver eye care services for cataracts, please contact Richard A. Levinson, M.D., to schedule an appointment.
What about Laser Cataract Surgery?
Good question. In 2013, FDA-approved Lasers became available for cataract surgery. These Lasers, called femtosecond lasers, can make the incisions involved in cataract surgery but they DO NOT remove the cataract. They do:
Make the small corneal incision for entering the eye.
Make the opening into the lens of the eye, called the capsulorhexhis.
They soften the lens, making it slightly easier to remove the lens with suction from the eye.
They can partially, but not precisely, make small incisions in the cornea to decrease astigmatism.
With Laser Cataract Surgery, the lens is still removed with phacoemulsification, ie breaking the lens into small fragments and using suction to remove the fragments from the eye. The Laser DOES NOT remove the cataract from the eye, and this is the most difficult step in cataract surgery. The Laser does make more precise, reproducible incisions than the incisions made by the surgeon manually, but the advantage is very minimal, especially in the hands of an experienced cataract surgeon.
The Laser is a small technological advance in cataract surgery, but at what cost? Presently, the femtosecond laser for cataract surgery adds $1000-$1500 to the cost of the procedure. This is an out-of-pocket expense not covered by insurance. There are some theoretical advantages to the more precise incisions made by the femtosecond Laser, but there is scant evidence that Laser-assisted cataract surgery is safer or provides better visual outcomes than traditional cataract surgery, in the hands of an experienced cataract surgeon. The femtosecond laser has limitations that compromise its efficacy in removing the cataract in the more difficult cases, such as when the patient has a small pupil that won’t dilate. And there are some complications associated with the Laser that are not present with non-Laser cataract surgery.
Less than 5% of cataract surgery in the U.S. today is performed with Lasers. I am not offering Laser cataract surgery to my patients, yet. There is no obvious advantage to the Laser, especially at the present cost. However, I think that the technological achievements of the Laser are impressive and will probably become more available as the price, hopefully, drops in the future and the technology continues to improve.
What is ORA Intraoperative Aberrometry?
Intraoperative Aberrometry, brand-name ORA, is a technology to measure, calculate and verify the accuracy of the intraocular lens, IOL, during cataract surgery. Once, again, this is an out-of-pocket expense, about $250 per eye and is not covered by insurance. In every cataract surgery today, the IOL power is always calculated pre-operatively with very accurate, laser-scanning measurements that are extremely precise. The ORA probably offers little advantage in routine cataract surgery, and I no longer find it to be useful.
What are the results of cataract surgery?
About 97% of patients have better vision after cataract surgery. Your vision may fluctuate for a month or so after surgery. After 3-4 weeks, you will be given a glasses prescription, if needed. If you need cataract surgery in both eyes, the second eye can be done within 1-2 weeks after the first eye, assuming the first eye is healing without problem.
Can cataracts recur?
No and yes. No, the cataract itself will not recur. However, when we remove your cataract, we leave the back capsular membrane of your old lens in place to support the new intraocular lens implant. If we didn’t leave this capsular membrane in place, there would be nothing to support the lens implant and it would fall back into the vitreous cavity, the back part of the eye. In approximately 50% of eyes following cataract surgery this capsular membrane will become hazy and interfere with vision. This opacified membrane, or “secondary cataract”, can easily be opened with a procedure called a YAG Capsulotomy. A YAG capsulotomy is a simple, painless, safe procedure that takes just a few minutes to perform. When we perform the YAG capsulotomy, we dilate the eye with an eye drop, that is all you will feel. The YAG Laser is then used to make a small, central opening in the hazy capsular membrane. You won’t feel anything during the YAG capsulotomy procedure. The vision will improve within hours after the YAG capsulotomy.
For the curious, YAG is an abbreviation for Yttrium, Aluminum and Garnet, the 3 metals used in producing the Laser energy. Actually, there is a fourth metal, neodymiun, that is also used, and the full name of the Laser is Nd:YAG Laser.
Do the lens implants ever wear out?
No. The lens implants are made of inert plastics that are extremely well-tolerated within the eye. They do not wear out and do not need to be periodically replaced.
Intraocular Lens
What Our Patients
are Saying
Google Maps Reviews – 4.8 out of 5 Stars
Mouse over or touch to Stop



The Fine Art of Vision Care

